Micrognathia and pierre robin sequence1/21/2024 
Guidelines for difficult airway management in neonatal cardiopulmonary resuscitation have not been established. Case 2 had 1p36 deletion syndrome complicated with PRS. Medical problems commonly caused by this anomaly include developmental delay, intellectual disability, seizures, vision loss, short stature, distinctive facial features, brain anomalies, orofacial clefting, congenital heart defects, and renal anomalies. 
1p36 deletion syndrome affects approximately 1 in 5000 newborns and is the most common terminal chromosomal deletion in humans. To our knowledge, there have been no reports on PRS patients experiencing severe dyspnea immediately after birth due to critical airway obstruction and who were rescued by fiberoptic nasotracheal intubation.Ĭase 2 had a diagnosis of 1p36 deletion syndrome with low anorectal anomaly, severe hearing loss, and hypoplastic auricle, in addition to the airway anomalies. In these cases, the tongue protruding into the nasal cavity occupied not only the pharynx, but also the nasal airway, resulting in severe dyspnea. Extreme posterior shifting of the tongue is considered an obstacle in fusion of the bilateral palate in the early fetal stage, resulting in a cleft palate. None of the four types in this classification was applicable to a novel type of our cases. Based on fiberoptic endoscopy, mechanism of upper airway obstruction in PRS is classified into four types according to position of tongue or palate attaching to pharyngeal wall. In our cases, micrognathia and an extreme type of glossoptosis resulted in severe airway obstruction and difficult oropharyngeal intubation at birth. Usually, progressive airway obstruction might become more noticeable in the second month of life. PRS refers to the association of micrognathia and glossoptosis and is characterized by varying degrees of upper airway obstruction, due mainly to glossoptosis. We reported two PRS cases that developed severe upper airway obstruction immediately after birth and were rescued by fiberoptic nasotracheal intubation. Subsequently, he underwent tracheostomy and is now under medical treatment at home. This clinical condition was considered an extreme type of glossoptosis and he was diagnosed as PRS. During the procedure of nasotracheal intubation, no complications or problems other than severe hypoxia were observed. 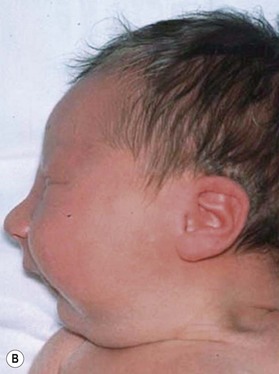
Because the urgent situation allowed us no time to prepare drugs, no sedatives were given. Before and during intubation, severe hypoxia (SpO2 < 80%) lasted, and insufficient spontaneous breathing with high concentration oxygen supply was only available treatment. Intubation was performed in supine position, and we carefully inserted a videoscope via a small interstice between the invaginated tongue and the pharyngeal wall. The endoscope fiber was 2.8 mm in outer diameter, and the intubation tube was 3.0 mm in inner diameter. Therefore, fiberoptic nasotracheal intubation was finally performed to secure the airway for resuscitation. Manual ventilation with high concentration oxygen or the use of nasopharyngeal airway was ineffective, and oropharyngeal intubation was impossible. Airway was completely obstructed, and the obstruction was not relieved by any change of position. Other physical examination findings were normal. He had micrognathia and cleft palate and his tongue protruded into the nasal cavity via a cleft palate as a result, only the backside of the tongue was visible by laryngoscopy (Figs. He developed severe dyspnea immediately after birth. No family history of congenital disorders was present. A 2574 g boy was born at 36 weeks gestational age by normal vaginal delivery after an uncomplicated pregnancy.
0 Comments
Leave a Reply.AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
